Three in four of the world’s new or emerging infectious diseases come from animals. Responsible for three million deaths a year, these diseases are largely transmitted through trading wildlife (legally and illegally) and factory farming.
Zoonotic diseases are appearing with increasing frequency. Swine flu and Covid-19 emerged in recent years, others that have emerged over past decades include SARS, MERS, Ebola and HIV – they all came from animals. The Covid-19 pandemic is the worst we have seen for generations. It is a warning of things to come if we don’t change the way we treat animals; as we continue to encroach on wildlife and expand factory farming, the threat of another pandemic increases.The next pandemic could be caused by a highly pathogenic bird flu virus with the potential to kill 60 per cent of those infected. Larger than any terrorist threat! It might be an antibiotic-resistant superbug that runs riot. It could be a new monkeypox variant or a completely new, previously unseen virus. It might be the resurgence of an old pathogen. It’s time to make the connections between eating meat and the destruction of wildlife, antibiotic resistance and disease outbreak. It’s time to end factory farming and go vegan.
Find out more about zoonotic diseases and how we can stop them
You may not have heard the word ‘zoonotic’ until recently, it sounds rather exotic! But did you know that measles, whooping cough, tetanus, polio, HIV and seasonal flu all came from animals? Recent infectious disease outbreaks such as SARS, MERS, Covid-19 and mpox are just a few more in a long line of zoonotic diseases but what concerns scientists is that they are now emerging with increasing frequency.
FAQs
What are zoonotic diseases?
Animals can sometimes carry harmful pathogens that can spread to people and cause illness – these are known as zoonotic diseases or zoonoses. Such diseases may be caused by viruses, bacteria, parasites or fungi. They may be mild or serious and in some cases, can cause death. Animals can appear healthy even when they are carrying an infectious agent, such as a virus for example, that can make people very ill. In fact, most natural hosts of zoonotic disease do not get ill, they may happily harbour the virus for their entire lives while displaying no symptoms.
How many people are affected?
Researchers estimate that based on the world’s current population and past pandemics, we can expect at least three million deaths from zoonotic diseases each year.
Globally, infectious diseases account for 16 per cent of all deaths but 44 per cent of deaths in low-resource countries.According to scientists, emerging zoonoses are responsible for some of the most high-profile and devastating epidemics, however, endemic zoonoses (such as mpox, for example) may pose a more insidious and chronic threat to both human and animal health.
How many zoonotic diseases are there?
Three out of every four new or emerging infectious diseases in people come from animals.
The World Health Organisation (WHO) says there are over 200 different zoonotic diseases that jump from animals to people. There may be a lot more to come; around 1.7 million viruses are thought to exist in mammals and birds and scientists say up to half of them may have the potential to spill over into humans.
WHO says: “During the past decades, many previously unknown human infectious diseases have emerged from animal reservoirs, from agents such as human immunodeficiency virus (HIV), Ebola virus, West Nile virus, Nipah virus and Hanta virus. In fact, more than three-quarters of the human diseases that are new, emerging or re-emerging at the beginning of the 21st century are caused by pathogens originating from animals or from products of animal origin”.Of course, there are already plenty of zoonotic diseases that are already causing untold misery. Of the 56 zoonotic diseases studied in the report Mapping of Poverty and Likely Zoonoses Hotspots, 13 of the most important were identified: zoonotic gastrointestinal disease, leptospirosis, cysticercosis, zoonotic tuberculosis, rabies, leishmaniasis (caused by a bite from certain sandflies), brucellosis (a bacterial disease that mainly infects livestock), echinococcosis, toxoplasmosis, Q fever, zoonotic trypanosomosis (sleeping sickness), hepatitis E and anthrax.
How do viruses and bacteria jump to humans?
Infections with zoonotic diseases may occur by direct or indirect contact. Direct infection can occur, for example, when a person comes into contact with contaminated saliva, blood, urine, mucous, faeces or other body fluids of an infected animal. This might occur when touching or handling animals or from bites or scratches. The pathogen (virus, bacteria, parasite etc) may enter the body via the inhalation of tiny respiratory droplets in the air or via the mouth, nose, eyes, open wounds, cuts or abrasions.
Indirect transmission may occur when people invade or disrupt the natural habitat of animals, picking up a pathogen from contaminated ground or plant foods, for example.
Transmission may also occur via food or water if they are contaminated with the faeces, urine or saliva of infected bats, birds or monkeys, for example. Vector-borne transmissions occur when a tick or an insect such a mosquito or flea, acquires a pathogen from an animal and then transmits it to a person by biting them.
Other factors contributing to disease emergence, including climate change, globalisation and urbanisation – most of these factors are caused by humans.
Why are zoonotic viruses a threat to humans?
Viruses are constantly evolving by mutating, mixing and matching their genes, sometimes with other viruses. A new strain of virus may be able to jump species and infect humans – like the coronavirus that caused Covid-19 – or the viruses that led to SARS, MERS, Ebola, HIV and many other zoonotic diseases.Professor Thomas Lovejoy, a senior fellow at the United Nations Foundation and professor of environmental science at George Mason University, said two to four new viruses are being created every year as a result of human infringement on the natural world, and any one of those could turn into a pandemic.
Why is animal agriculture to blame?
Human activity and the expansion of animal agriculture to meet the world’s insatiable hunger for meat has changed three-quarters of the planet’s surface, squeezing wildlife into ever-smaller corners while large-scale factory farms expand.
Agricultural intensification and expansion play a major role in pathogen emergence. Factory farms provide the ideal environment for disease spillover from wild animals into livestock or for emerging viruses to take hold and spread. Nipah virus emergence in Malaysia, for example, occurred on a large pig farm surrounded by mango trees and set on the edge of native forests. This created favourable conditions for spillover of Nipah virus from bats to pigs and from pigs to people. Large pig and poultry farms, warn scientists, provide the ideal environment for the genetic mixing of viruses needed to source a future pandemic flu strain. We have been warned.
It’s not just new diseases that we should be worried about. Scientists also warn that evidence from the hundred or so largest zoonotic outbreaks over the past 30 years points to agricultural intensification as a primary driver of the resurgence of older pathogens such as anthrax, brucellosis and salmonellosis.
Our relationship with animals can no longer be just focused on exploitation, as scientists say that the way meat is produced is now considered to be a global threat. It’s not just a case of banning wet markets, although that can’t come soon enough – we need to stop factory farming too. Intensive farming allows viruses and bacteria to easily spread and mutate in overcrowded, densely populated sheds. Animal agriculture lies at the heart of future pandemic threats.
We need to stop deforestation and tackle the illegal wildlife trade, the fourth most common crime committed worldwide. We are decimating wild landscapes, killing wild animals or caging them and sending them to market. Invading and disrupting ecosystems will inevitably shake viruses loose from their natural hosts.Head of the UN Environment Programme (UNEP), Inger Anderson says “As we continue to encroach on fragile ecological ecosystems, we bring humans into ever-greater contact with wildlife. Further, illegal wildlife trade and illegal wet markets are not infrequent causes of such diseases. Around 75 per cent of new and infectious diseases are zoonotic and, in fact, about 1 billion cases of illness and millions of deaths occur every year from these diseases”.
Why do factory farms spread disease?
Scientists have been warning about the health risks posed by intensive factory farms for years, including the opportunities they provide for viruses and bacteria to spread and mutate.
As factory farming spreads across the globe, diseases follow, spreading like wildfire through the densely populated sheds. Ninety per cent of farmed animals across the world are now kept in factory farms. Animals kept in horrific conditions are more susceptible to disease due to the extreme stress they experience from their cramped and inhumane surroundings. Bred for fast growth, their immunity is low. It’s a perfect storm of our own making.
Huge intensive poultry farms provide the perfect breeding ground for a mutating virus. Chickens are raised in closed, filthy, stressful and crowded, industrial facilities with little or no natural light, this is important as ultra-violet (UV) light harms viruses. We are literally handing the bird flu virus, for example, the perfect opportunity to mutate into a more deadly form, to do its worst!
Pig farming has also changed dramatically in recent decades and scientists warn that there are many reasons to expect that pigs will increase in importance as vectors of pandemic threats. Scientists consider pigs to be ideal ‘mixing vessels’ for the development of new viruses because they are susceptible to flu viruses from pigs, humans and birds.It’s high time we start considering the fact that our increased consumption of meat and dairy foods isn’t just wreaking havoc on our health and the environment, it’s sparking pandemics that kill thousands, potentially millions, of people. Some highly-pathogenic strains of viruses may be poised, ready to cause the next pandemic in humans. End factory farming before it ends us!
What is a wet market?
It’s thought that the virus that causes Covid-19 came from a food market in China that sold wild animals. Such markets are filled with a mixture of domestic and wild animals including poultry, civet cats, snakes, pangolins, bats, beavers, foxes and dogs to name just a few. Some found in the markets may have been captured illegally in the wild.
Some viruses can be spread through inhaling tiny respiratory droplets of virus in the air or from picking up the virus on your hands from surfaces then touching your mouth, nose or eyes. They may be carried in the saliva, blood, urine, mucous, faeces or other body fluids of an infected animal or person. The dreadful, cramped conditions and mix of wild and domestic creatures, alongside the throngs of people is a pandemic in the making.
Imagine a market, with cages of different animals stacked on top of each other with people packed in too. Animals being slaughtered, skinned, chopped up and handled – you could hardly make a more perfect breeding ground for an emerging virus!As industrialised farming has expanded in China, small-scale farmers have moved over to the wildlife market and have been geographically pushed too into remote areas inhabited by bats. This is just one of the many reasons why factory farming is as much to blame.
What is the link between bats, pangolins and Covid-19?
The virus that causes Covid-19 is 96 per cent identical to a bat coronavirus, suggesting that bats are the natural host. Reclusive and nocturnal – bats are not to blame, we are! Bats have been harbouring such viruses for thousands of years, if not longer. Trading in bats at wet markets and hunting and eating them as bushmeat (see Ebola) has brought them into close contact with people. It’s like sticking your hand in a pan of boiling water and blaming the water!
Some scientists think that the Covid-19 virus may have passed to humans from bats via another animal, what’s called an intermediary host. Initially, snakes and bamboo rats were favoured candidates, however, research suggests that it may have come to humans from pangolins or some other animal.
Pangolins are an endangered wild animal, eaten as a delicacy in many parts of the world, they are the most trafficked animals on the planet. While the specific source remains uncertain, it is clear that the virus that causes Covid-19 came from human interaction with wildlife.Scientists have previously warned that bat viruses can infect humans and that this could be a problem. In 2016, a bat virus similar to the one that caused Covid-19 was described as being ‘poised for human emergence’. After Covid-19, many people said they wanted things to go back to ‘normal’ but it is ‘normal’ that got us here!
Where did SARS come from?
SARS also came from a bat virus but human infection was via civet cats which were caught in the wild and transported to markets for food.
The 2003 severe acute respiratory syndrome or SARS outbreak was the first global pandemic of the 21st century. It began in late 2002, when cases of a mystery pneumonia-like illness began occurring in people in Guangdong province in China. The outbreak was brought under control in July 2003 with 8,098 reported cases and 774 deaths. Around 10 per cent of those infected with the disease died.
China, Hong Kong and Taiwan were the worst affected countries, although the virus also spread to Canada, where there were 251 cases. In the UK, four cases were recorded with no deaths.
When viruses jump from wildlife to humans, it is often as a result of their natural host’s habitat being disturbed. Due to human activities, the SARS virus is thought to have expanded its host of infection, first to civet cats and then to humans. The virus jumped from horseshoe bats in a remote area of Yunnan province in China to civet cats which were then transported to markets and restaurants in Guangdong, leading to the SARS outbreak in humans.
Markets became heavily contaminated, along with civet cats, other animals that tested positive for the SARS virus included domestic cats, red foxes, lesser rice field rats, geese, Chinese ferret-badgers and wild boar.The bat cave where the SARS viruses were found is just one kilometre from the nearest village. In 2017, scientists warned: “The risk of spillover into people and emergence of a disease similar to SARS is possible”. The warnings were ignored.
Where does MERS come from?
Middle East respiratory syndrome or MERS is caused by a coronavirus thought to have spilled over from bats into camels, in which is it now endemic. First detected in a person in Saudi Arabia in 2012, it’s thought that MERS viruses have been circulating among camels since the early 1980s if not earlier. Like Covid-19, the MERS virus causes respiratory infection in humans, ranging from asymptomatic to severe pneumonia. The virus only causes a mild infection among camels but spreads easily between them.
Camels are raised for milk, meat, fibre (wool and hair) as well as transport and racing. Owing to substantial governmental support, camel farming and racing competitions have expanded hugely, worsening the desertification that led to the banning of free grazing in 2005. As a consequence, camels are now frequently housed in compact barns alongside workers. High-density farming combined with the increased movement of camels for racing and breeding, have increased their exposure to humans, driving the spillover of the MERS virus from camels to humans.
MERS kills around 34 per cent of people infected. Between 2012 and 2019, around 2,500 cases of MERS and over 900 deaths were recorded. There is no vaccine and cases continue to appear. Since MERS was first identified in 2012, over 2,600 cases have been detected in 27 countries. In Europe, eight countries have reported confirmed cases, all with direct or indirect connections to the Middle East. Most cases continue to be reported from the Middle East. Since the beginning of 2022, and as of 3 May 2022, two MERS cases have been reported in Qatar, including one death.Like Covid-19, MERS causes more severe disease in people with underlying conditions such as diabetes, kidney problems, chronic lung disease and compromised immune systems. The World Health Organisation says that people with underlying medical conditions should avoid contact with animals, particularly camels. General hygiene measures, such as regular hand washing before and after touching animals and avoiding contact with sick animals, are recommended. They also say food hygiene practices should be observed and that people should avoid eating meat that has not been properly cooked and not drink raw camel milk or camel urine! We could just stop farming and racing camels.
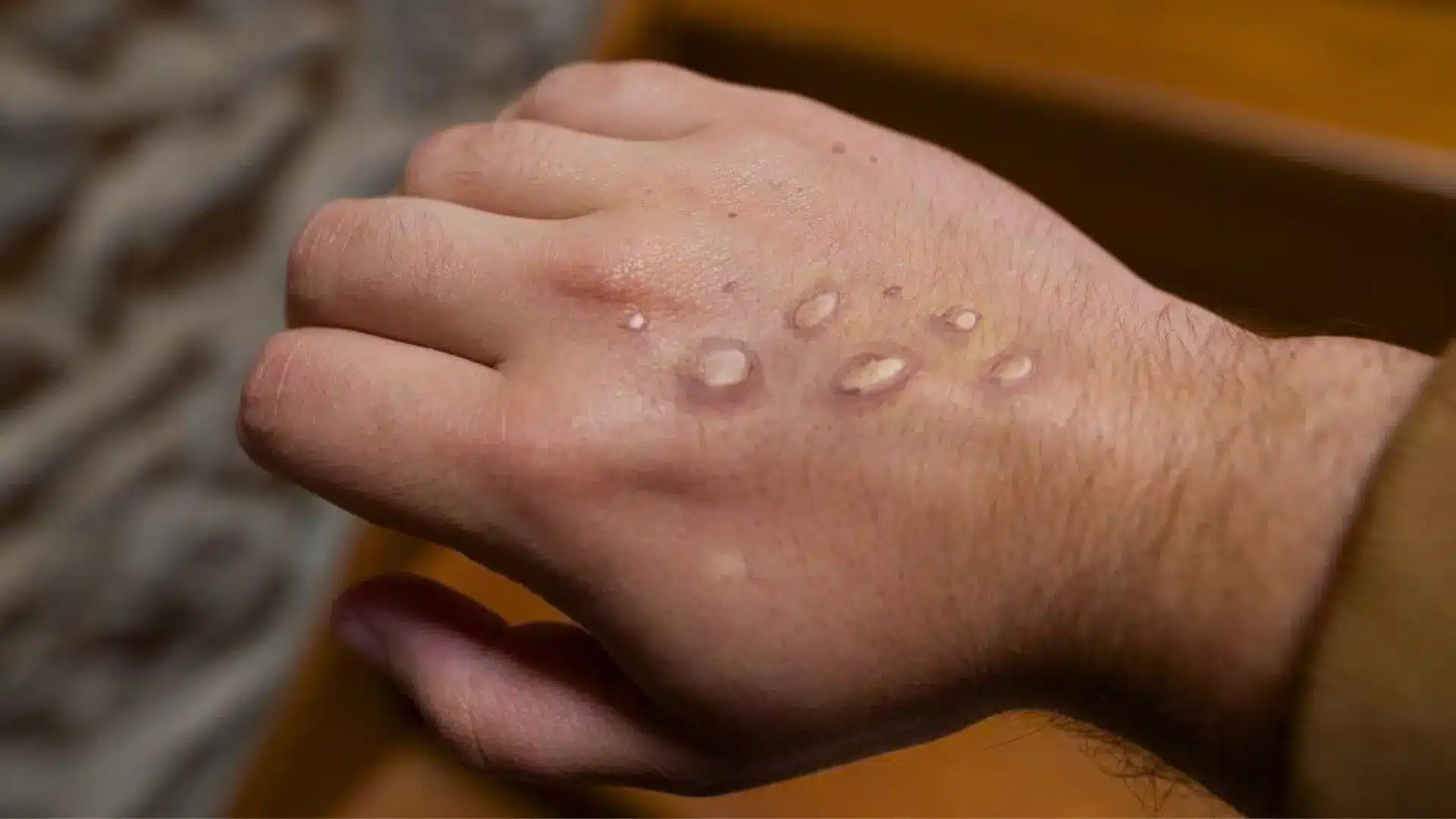
What is mpox and where did it come from?
Mpox (previously known as monkeypox) is a zoonotic infectious disease with symptoms similar to those seen in people with smallpox, although less severe with a case fatality rate of around three to six per cent.
The disease was first seen in captive monkeys in a research laboratory in Denmark in 1958. Infections have occurred in squirrels, rats, mice, monkeys, prairie dogs and humans. However, its natural hosts are squirrels and other rodents and it spreads in areas where they are hunted by people for meat. Human infection occurs most frequently in small villages where people hunt and eat squirrels and other small mammals. People usually catch the disease from hunting and handling dead animals (bushmeat), animal bites or scratches, body fluids, contaminated objects or close contact with an infected person, as is the case for some travellers. This virus is endemic to western and central Africa, outbreaks in other countries tend to be related to the exotic pet trade and international travel.
It’s another classic case of humans’ interference with wild animals shaking a virus lose from its natural host! We are decimating wild landscapes, killing wild animals or caging them and sending them to market, invading and disrupting ecosystems – Covid-19 was a warning shot that we seem to have learned nothing from.
The first human case of monkeypox was recorded in 1970 in the Democratic Republic of the Congo. A few thousand cases a year are thought to occur in Africa, typically in the western and central parts of the continent. Cases outside Africa have previously been limited to a handful that were associated with travel to Africa or with the importation of infected animals.
In May 2022, outbreaks were reported across many non-endemic countries, mainly in Europe (the UK, Spain, Portugal, Germany, Belgium, France, the Netherlands, Italy, Sweden) but also in the US, Canada, Australia and the United Arab Emirates (UAE).
On 23 July 2022, the World Health Organisation (WHO) declared the outbreak a public health emergency of international concern (PHEIC), stating that “we have an outbreak that has spread around the world rapidly, through new modes of transmission, about which we understand too little”. A global response to the outbreak included public awareness campaigns to reduce the spread of the disease and repurposing of smallpox vaccines.
In May 2023, WHO declared an end to the PHEIC, citing steady progress in controlling the spread of the disease. Relatively low levels of cases continued to occur and as of 8 March 2024, there have been a total of 94,766 confirmed cases and 182 deaths in 117 countries. This number of cases (detected outside of Africa) has surpassed the total number detected outside the continent since 1970.
Our relationship with animals can no longer be based on exploitation, using animals for food, clothing, entertainment and as commodities is increasingly becoming a global threat to health. It’s time to go vegan.
Find out more about monkeypox here.
When did bird flu start?
A classic example of a zoonotic disease. Avian influenza became commonly known as bird flu in the late 1990s when there were several deaths in Hong Kong.
The H5N1 avian influenza virus has been infecting poultry and other land birds since the 1950s but in 1996 a highly pathogenic strain of H5N1 spread among farmed geese in a small town 50 miles outside the capital of Guangdong killing more than 40 per cent of the birds it infected.
By 1997 the virus had spilled over into poultry farms and live-poultry wet markets in Hong Kong, killing large numbers of birds. It also infected 18 people and six died – the first known case of H5N1 in humans. Infections in people occurred directly from contact with chickens, so to stop the outbreak, the government ordered the slaughter of more than 1.5 million chickens.In 2001, the number of chickens dying in retail markets throughout Hong Kong attracted attention, H5N1 viruses were again isolated and the government carried out a second territory-wide slaughter of chickens. During the subsequent 2005 outbreak, tens of millions of chickens and other poultry in south-east Asia were again slaughtered in an effort to contain the disease. It continues to appear with deadly consequences.
What are the origins of bird flu?
A virus has one job – to infect animals or plants and make more copies of itself. If a random mutation occurs that makes this easier, the mutated version will thrive. Live markets and factory farms provide a perfect breeding ground for the emergence of new viruses, including bird flu.
Wild waterbirds, such as ducks, geese, swans, gulls, terns and shorebirds are the natural hosts of bird flu viruses in which they occur without making them ill, and have done so for millions of years. Viruses are passed on in water from one bird to another but are not problematic. In waterbirds, the avian influenza viruses had an ideal environment in which they could co-exist without harming the host. However, when these birds were taken to market, the virus could no longer spread from bird to bird in water so had to mutate or die. In this new, stressful environment, mutations occurred and enabled the virus to spread. Commercial poultry farms, wet markets, poultry slaughtering facilities, pig farms, human dietary habits and the global trade in exotic animals are all now implicated in the spread of influenza viruses.
Bird flu is causing increasing levels of illness and death in large numbers of land birds, especially poultry. Factory farms make it easy for these viruses to mutate and spread. These viruses are changing and beginning to jump species with increasing frequency, infecting different animals, including pigs, whales, horses, seals, dogs and humans. In 2003-2004 a number of captive tigers and leopards in a zoo in Thailand who were fed fresh chicken meat died of H5N1 infection. In 2006, H5N1 was isolated from a domestic cat found dead on the northern island of Ruegen in Germany, where more than 100 wild birds had died from H5N1.
In 2024, dairy cows in several states in America were found to be infected with H5N1. It remains unclear how they were infected as most infected carnivorous mammals are thought to have got the virus from eating dead infected birds.
The pattern of infection in recent years, with different animals and humans affected, represents a disturbing development. It may be entirely possible that a natural chain of mutations could lead to a bird flu virus acquiring the capability of airborne transmission between people. Some of these mutations have already happened and scientists say we may be just three more mutations away from a pandemic.
This could lead to a human pandemic that would circle the world in weeks. If and when an influenza pandemic arises from one of the currently circulating, highly pathogenic strains, the death rate would be devastating.
World Health Organisation spokesman for the Western Pacific region, Peter Cordingly, says: “…the bottom line is that humans have to think about how they treat their animals and how they farm them, how they market them – basically the whole relationship between the animal kingdom and the human kingdom is coming under stress”.For more information see bird flu.
Why was the Spanish flu pandemic so deadly?
Around a third of the world’s population, up to 500 million people, are thought to have been infected during the Spanish flu pandemic of 1918. One of the deadliest pandemics in human history, estimated to have killed up to 50 million worldwide. The estimated number of infections and deaths varies widely but it was at least 10 times more deadly than seasonal flu (which kills around 0.1 per cent), killing from one per cent to 2.5 per cent or higher of those infected.
Spanish flu is so-called because when the outbreak occurred, wartime censors in Germany, France, the UK and the US played down early reports of the illness to hide the devastating effects it was having on people in their countries. Spain was not involved in the war and had no such censorship, so appeared to be hit harder than other places. It remains unclear where the pandemic actually started, some say Kansas, others suggest Northern France or even China. Regardless of where it started, the outbreak spread rapidly across the world affecting many soldiers who fought during the First World War.
The majority of those who died were young, healthy adults aged between 15 and 44. Most perished as a result of secondary infections such as bacterial pneumonia. Many factors contributed to the pandemic’s lethal impact, as soldiers from almost every country in the world came together to endure the horrors of war – stress, fear, cold weather, crowded conditions and poor hygiene. A recipe for disaster not unlike a factory farm!
Which specific animal the 1918 pandemic influenza virus came from is unknown but it was caused by an H1N1 virus with genes of avian origin. One theory is that the virus infected humans directly from birds before the pandemic and that it adapted or mutated in humans into the one causing the outbreak. In other words, it evolved via the mixing of bird and human viruses in human hosts. Another study suggests that the ‘parent virus’ went from humans to birds then back to humans in a more lethal form.
Scientists say the virus could have jumped to humans from birds via pigs which are so susceptible to infection with influenza viruses, from humans, birds and pigs, that they have been referred to as ‘mixing vessels’. An outbreak of a flu-like illness in pigs occurred in the US at the same time as Spanish flu emerged, but it’s unclear in which direction the illness spread as human-pig transmission is also possible!
However the virus emerged, one thing is clear, it was the deadly product of viral evolution and the close mixing of people with animals.Influenza viruses generated in pigs or transmitted between birds and humans clearly pose a serious threat to millions of people.
What caused the Asian flu pandemic?
The 1957 Asian flu pandemic was caused by an H2N2 virus originating in China in early 1956 that is estimated to have killed around 1.1 million people. The origin of the virus is unknown but scientists think it may have come from one in wild ducks combining with a human strain, again possibly with pigs acting as an intermediary ‘mixing’ host bridging the gap between birds and humans. While H2N2 has disappeared from humans, it persists in wild and domestic birds (chickens, guinea fowl and ducks). Re-emergence of this virus in humans is a significant threat due to the absence of immunity in people under 50.
What caused the Hong Kong flu pandemic?
The 1968 Hong Kong Flu pandemic resulted in an estimated one million global deaths. It was caused by an H3N2 virus descended from the H2N2 virus that caused the 1957 pandemic. The virus contained a mixture of genes from a low-pathogenic avian influenza virus and some from the H2N2 virus that had been circulating in people since the 1957 pandemic. Again, while H2N2 and H3N2 are undoubtedly of avian – possibly wild duck – origin, a potential role for pigs cannot be ruled out and the ‘mixing vessel’ hypothesis may explain how these zoonotic pandemic-causing diseases emerged.
What caused the 2009 swine flu pandemic?
The 2009 flu pandemic was caused by an H1N1 virus from pigs, it was first detected in Mexico and then spread quickly across the world. The so-called ‘classical swine H1N1’ virus, containing elements of human, pig and bird viruses, emerged and became predominant among North American pigs during the late 1990s.
The mixing of live pigs from Eurasia and North America through international trade then created the opportunity for viruses from the different pigs to mix giving rise to the 2009 H1N1 virus which scientists call a ‘quadruple reassortant’ virus because it contains elements originating from humans, birds, North American pigs and Eurasian pigs.
This new virus, containing a unique combination of influenza genes, primarily affected children and younger adults as many older people turned out to be immune. The number of deaths during the first year the virus circulated is estimated to be between 151,700 and 575,400.It is now one of the seasonal flu viruses that circulate each winter. If you’ve had flu in the last few years, there’s a chance it was caused by this virus.
Why is bird flu such a danger to humans?
Avian influenza (bird flu) is a particular concern to scientists who think it may be the cause of the next global pandemic.
The H5N1 virus, for example, is concerning many scientists as the mortality rate in humans is a terrifying 50 per cent or higher – seasonal flu kills about 0.1 per cent of those infected. Tens of millions of birds have died of H5N1 influenza and hundreds of millions of chickens, ducks, turkeys and geese have been slaughtered and disposed of, to limit the spread of H5N1.
Most cases of infection in humans have involved people handling, slaughtering or consuming infected poultry. Since 2003, nearly 900 people have been infected with the H5N1 avian influenza viruses in 23 countries and over 463 of them have died, with fatalities in Indonesia, Egypt, Vietnam, China, Cambodia, Thailand and Canada. These numbers might seem low, compared with other pandemics, however, if the virus changes to become more easily spread between humans, we could be facing a deadly pandemic the likes of which we have never seen before.
Highly pathogenic versions of H5N1 have spread from Asia to Europe and Africa, resulting in millions of poultry infections. Strains of the virus can become more deadly when they mutate in factory farms. These can then pass back to wild birds. Migrating waterfowl – wild birds, including shorebirds and gulls, as well as domestic ducks are considered to be the natural reservoir of the virus and may then spread the more deadly strains around the world. These animals may carry and shed viruses without showing any signs of illness – they become ‘silent carriers’, sustaining and perpetuating H5N1 and transmitting it to other susceptible hosts.
The global spread of H5N1 is considered a significant pandemic threat. If the virus mutates to become more easily transmissible, David Nabarro, one of the most senior public health experts at the World Health Organisation, says the “range of deaths could be anything between five and 150 million”. So far, there have been a handful of person-to-person cases. However, influenza viruses constantly undergo genetic changes, it would be an extremely serious cause for concern if H5N1 become more easily transmissible among humans.
H7N9 is another virus with pandemic potential. First detected in poultry in China in 2013, the number of human cases has exceeded 1,500 and over 600 people have died. Most H7N9 infections in people result from contact with infected poultry, especially in markets where live birds have been sold, or by having contact with places where infected poultry have been kept or slaughtered. Again, infections don’t cause severe disease in poultry, so the virus can spread silently and is now ubiquitous in Chinese poultry. Like H5N1, a small number of cases may have spread from person to person but generally, H7N9 doesn’t spread easily between people. Virologist Professor Yoshihiro Kawaoka of the University of Wisconsin said: “If H7N9 viruses acquire the ability to transmit efficiently from person to person, a worldwide outbreak is almost certain…”.
These are just two of many bird flu viruses of concern, there are many others! In 2018, a new influenza virus, H7N4, emerged when it was detected in a 68-year-old woman hospitalised in Jiangsu province in eastern China. She had been handling live poultry. This was the first recorded case of this virus infecting a human showing how unpredictable viral evolution in livestock can be.
Bird flu has gone from being a relatively rare occurrence to one that crops up frequently and Uganda has not escaped. In early January 2017, outbreaks of H5N8 were reported for the first time in wild and domestic birds along the shores and on some islands of Lake Victoria, in central-southern Uganda.
As we have seen with Covid-19, when a new infectious virus emerges, it’s not just people going to wildlife markets that die – it’s office workers in New York, engineers in Zimbabwe, commuters in London, shopkeepers in Italy and students in Madrid. They are joined by people in every city, town and village around the world, dying after shaking someone’s hand, touching their face or simply breathing in, in the wrong place at the wrong time. One way to take control of the situation would be for huge numbers of people to stop eating poultry, pigs and other animals and remove the viral reservoir of factory farms. It’s time to end factory farming before it ends us.For more information see bird flu.
Where did EBOLA come from?
Ebola is one of the world’s deadliest infectious diseases; the case fatality rate is around 50 per cent but has varied from 25 to 90 per cent in past outbreaks. It is another zoonotic disease, bats are the most likely natural host but the virus can be caught from other animals such as monkeys and chimpanzees.
This viral haemorrhagic fever in humans and other primates is caused by ebolaviruses transmitted to people from wild animals and spread through human-to-human transmission. It was first identified in 1976, in two simultaneous outbreaks, one in Nzara in South Sudan and the other in a village near the Ebola River called Yambuku in the Democratic Republic of the Congo.
The 2014-2016 outbreak in West Africa began in a small village in Guinea with the infection of a young boy who had been playing in a hollow tree housing a colony of fruit bats. His death was followed by that of his older sister and then his mother. The virus soon spread to Guinea’s capital city. Ten days later, with 49 confirmed cases and 29 deaths, the WHO officially declared an outbreak of Ebola. Two and a half years later, with widespread transmission to Guinea, Liberia, and Sierra Leone plus a handful of cases in Europe and the US, the outbreak ended with more than 28,600 cases and 11,325 deaths.
The virus spreads through direct contact with body fluids, such as blood, saliva, mucus, vomit, faeces, breast milk, urine and semen from infected humans or other animals. Fruit bats are believed to be the natural host, able to spread the virus without being affected by it. It can infect humans by entering the body via the nose, mouth, eyes, open wounds, cuts and abrasions. Besides bats, other wild animals sometimes infected include several monkey species, chimpanzees, gorillas, baboons and duikers (forest antelope).
Bushmeat is the name for any wild animal that is killed for consumption including antelopes, chimpanzees, rats, porcupines, snakes and fruit bats. The use of bats as food raises particular concern, as bats host more zoonotic viruses than most other animals, including rodents. In Africa’s Congo Basin, people eat an estimated five million tonnes of bushmeat per year, according to the Centre of International Forestry Research. Dr Olivier Restif from the University of Cambridge found that the scale of the bat bushmeat trade in Ghana was much higher than previously thought, with more than 100,000 bats killed and sold every year.
Hunting, butchering and eating wild animals can lead to the transmission of zoonotic diseases through animal bites, scratches, body fluids, tissues or faeces. Because the world’s population is expanding, close contract with wildlife has increased, this is often the first driver of emerging diseases. Deforestation is also a major contributor to recent outbreaks and cases of Ebola have often been close to recently deforested land.“The Ebola outbreak is an opportunity to clamp down on a practice which both causes disease outbreaks and empties forests of wildlife. At a minimum, governments should zealously enforce bans on the hunting and consumption of bats and apes.
Where did HIV/AIDS come from?
The human immunodeficiency virus (HIV) is another zoonotic disease – the virus jumped from primates to humans.
Since the beginning of the epidemic, 86 million people have been infected with the HIV virus and about 40 million people have died of HIV. Globally, 39 million people were living with HIV at the end of 2022.
There are two main types of virus, HIV-1 and HIV-2, both derived from simian immunodeficiency viruses (SIVs) that circulate in over 40 species of African non-human primates. Most SIVs infect monkeys and have been circulating in different species, causing them no problems, for many years.
HIV-1 is the most prolific but HIV-2 is most common in western Africa and is becoming more common in India. HIV-1 is a mutated version of a chimpanzee virus, which probably made the species jump to humans as a result of chimpanzees being hunted and eaten. Like humans, chimpanzees are apes and it is assumed they acquired SIVs from monkeys, probably by predation. Scientists think the jump from chimpanzees to humans happened in the 1920s, in what is now the Democratic Republic of Congo. HIV-2 comes from sooty mangabey monkeys and the crossover to humans in the 1960s is believed to have happened in a similar way, through the butchering and consumption of monkey meat.
When habitats of wild animals are disturbed by humans, viruses that they are natural hosts to can jump host, as exemplified by the story of the HIV virus from chimpanzees in rainforests of West Africa. It’s the same story being replayed around the world with different host species and different viruses, the only constant is humans, disturbing the equilibrium at our peril.AIDS has become one of the most devastating infectious diseases to have emerged in recent history. HIV and AIDS continue to be a major global public health issue.
What is the Nipah virus?
The Nipah virus is a highly pathogenic virus that can spread from animals, such as fruit bats and pigs, to humans.
Infection may cause no symptoms, mild symptoms such as a cough, headache and breathlessness or extreme acute respiratory infection and fatal encephalitis (inflammation of the brain). It is estimated that 40 to 75 per cent of those who are infected die.
Fruit bats are the natural host of this virus but pigs may become infected, possibly by eating fruit contaminated with bat secretions, and the virus is highly contagious among pigs. It was first identified in a 1999 outbreak among pig farmers in Sungai Nipah, a village in Malaysia. The outbreak caused a relatively mild disease in the pigs, but nearly 300 human cases with over 100 deaths were reported. In order to stop the outbreak spreading, more than a million pigs were killed. Subsequent outbreaks have occurred in India and Bangladesh with the latter experiencing outbreaks most years.
There are currently no specific drugs or vaccines for Nipah virus infection. In 2019, Richard Hatchett, chief executive of the Coalition for Epidemic Preparedness Innovations said: “Twenty years have passed since its discovery, but the world is still not adequately equipped to tackle the global health threat posed by Nipah virus”.WHO say that if a Nipah virus outbreak is suspected, animal premises should be quarantined and culling of infected animals, with close supervision of burial or incineration of carcasses, may be necessary to reduce the risk of transmission to people. Or we could just stop pig farming!
Did measles come from animals?
The measles virus emerged as a zoonotic disease from the rinderpest virus that caused ‘cattle plague’ around the 11th to 12th centuries when humans were living close to cattle infected with this virus. In June 2011, the United Nations FAO confirmed rinderpest virus was eradicated, but measles remains.
We learned about the R number during the Covid-19 pandemic; it refers to the average number of people an infected person passes the infection on to. For the common cold, it is two to three, for seasonal flu, the number is 0.9 to 2.1 but for measles, on average, each person infected infects 12 to 18 (susceptible or unvaccinated) people, making it one of the most infectious diseases known.
It can lead to serious and potentially life-threatening complications including pneumonia and encephalitis. According to the World Health Organisation (WHO), more than 140,000 people died from measles globally in 2018 – most of them children under the age of five, despite the availability of a safe and effective vaccine.
Around one in five children with measles experience complications such as ear infections, diarrhoea and vomiting, pneumonia, meningitis and eye disorders. One in 10 children with measles ends up in hospital. There is no treatment, vaccination is the only way of preventing it. Director-General of the WHO, Tedros Adhanom Ghebreysus, says: “The fact that any child dies from a vaccine-preventable disease like measles is frankly an outrage and a collective failure to protect the world’s most vulnerable children”.Measles is extremely contagious and should be taken as a warning of how highly infectious zoonotic diseases can be.
Why are antibiotic-resistant superbugs a problem?
Antibiotics have been helping us fight infection since the 1940s. Before that, even a small scratch could be fatal. Giving birth and having surgery were a lot riskier and sexually transmitted infections (STIs), such as syphilis and gonorrhoea, caused untold misery and could be a death sentence.
The overuse of antibiotics, in people and farmed animals, has led to the emergence of antibiotic-resistant superbugs. If antibiotics fail, chest infections, urinary tract infections (UTIs), cuts, insect bites and even small scratches could develop into sepsis (blood-poisoning) which can be fatal if not treated quickly. In the UK, five people die from sepsis every hour and the number is rising.
The UK Sepsis Trust CEO, Dr Ron Daniels, says: “…nearly 40 per cent of E. coli – the bacteria that causes a huge number of infections – is now resistant to antibiotics and these organisms account for up to one third of episodes of sepsis, showing the vital need for responsible use of antimicrobial drugs”.
The idea of dying from a horsefly bite is unthinkable but is fast becoming a possibility, thanks to the overuse and abuse of antibiotics. Professor Colin Garner, chief executive of Antibiotic Research UK, says: “Now we are in real danger that we could return to a pre-antibiotic past, where dirty wounds, bites and conditions like TB and typhoid might kill”.The World Health Organisation (WHO) says that antibiotic resistance is one of the biggest threats to global health, food security and development today.
Where do superbugs come from?
Superbugs or antibiotic-resistant bacterial infections result from the overuse of antibiotics. An incredible 73 per cent of the world’s antibiotics are used in animal agriculture, not for treating diseases in humans. So as well as new emerging viruses coming from factory farms or wild animals taken to markets, we have the serious global threat of antimicrobial resistance (AMR).
Antibiotic use in livestock outweighs human consumption in many countries, in the US, for example, 80 per cent of all antibiotics are used in animals. The UK government says: “As in humans, the sub-optimal use of antimicrobials in agriculture and veterinary practice contributes to the rise and spread of AMR all over the world”.
Scientists warn that the 1.3 million global deaths caused by AMR each year could rise to 10 million by 2050 if no action is taken. That means AMR could kill more people than cancer.
Due to the increasing global demand for meat, it’s predicted that antibiotic use in cattle, chicken and pigs worldwide will increase by eight per cent by 2030. There have been some improvements, in some countries, but it could be that the action being taken to reduce antibiotic use in humans and animals is too little, too late!
Colistin, described as a ‘last resort’ antibiotic for humans, is still used widely in livestock, especially pigs, in some parts of the world and in 2015, bacteria from pigs carrying colistin-resistance genes were identified in China. Colistin-resistant bacteria have now been identified in bacteria infecting farmed animals all over the world.
Scientists point out the stark parallels between the AMR crisis and the climate crisis – both driven by the increasing global demand for cheap animal foods. The WHO talk about a ‘One Health’ solution because AMR does not recognise geographic or human-animal borders – we all share one planet. The most effective way to tackle antibiotic resistance is to change the way we live and eat, reducing antibiotic use in humans and animals.
The contribution from agriculture to AMR is significant and growing. Of course, livestock industries are inevitably resistant to change but the obvious solution is to drastically reduce consumption of animal foods. The widespread adoption of a vegan diet would remove the factory farms that are the breeding grounds for these superbugs.
AMR is a problem of our own making, in humans, and in animals as a direct consequence of the inappropriate use of antibiotics in a drive to produce cheap meat, fish and dairy foods on an industrial scale. Failure to act may result in the chilling prospect of an apologetic doctor saying to you: “Sorry but there’s nothing we can do for you”.Neither viruses nor bacteria respect international borders so going vegan is the clear solution.
How do we prevent future pandemics?
Every few years or so, for a number of decades now, viruses from wild animals have been emerging, including Marburg virus causing haemorrhagic fever in 1967, Ebola virus causing haemorrhagic fever in 1976, Hendra virus causing severe pneumonia in 1994 and Nipah virus causing neurological and respiratory diseases in 1998. All passed to people via intermediary hosts – wildlife or farmed animals exploited and killed by people.
Preventing future outbreaks could be achieved by adopting an approach that considers both natural and social aspects of where diseases come from. This means monitoring what viruses are present in nature but more importantly, governments need to issue laws and policies to protect wildlife and prohibit consumption of wild animals. And to end animal agriculture – including, with urgency, to end factory farming.
Most of the viruses causing new infectious diseases have been traced to factory farms, slaughterhouses, wildlife markets and the legal and illegal wildlife trade.Professor Diana Bell and colleagues from the United Kingdom’s University of East Anglia’s School of Biological Sciences warns: “A major lesson from SARS is that the underlying roots of newly emergent zoonotic diseases may lie in the parallel biodiversity crisis of massive species loss as a result of overexploitation of wild animal populations and the destruction of their natural habitats by increasing human populations”.
What can we conclude?
Every few years or so, for a number of decades now, viruses from wild animals have been emerging, including Marburg virus causing haemorrhagic fever in 1967, Ebola virus causing haemorrhagic fever in 1976, Hendra virus causing severe pneumonia in 1994 and Nipah virus causing neurological and respiratory diseases in 1998. All passed to people via intermediary hosts – wildlife or farmed animals exploited and killed by people.
Preventing future outbreaks could be achieved by adopting an approach that considers both natural and social aspects of where diseases come from. This means monitoring what viruses are present in nature but more importantly, governments need to issue laws and policies to protect wildlife and prohibit consumption of wild animals. And to end animal agriculture – including, with urgency, to end factory farming.
Most of the viruses causing new infectious diseases have been traced to factory farms, slaughterhouses, wildlife markets and the legal and illegal wildlife trade.Professor Diana Bell and colleagues from the United Kingdom’s University of East Anglia’s School of Biological Sciences warns: “A major lesson from SARS is that the underlying roots of newly emergent zoonotic diseases may lie in the parallel biodiversity crisis of massive species loss as a result of overexploitation of wild animal populations and the destruction of their natural habitats by increasing human populations”.
What can we conclude?
Experts have been warning us about this for years. Most of the viruses causing new emerging diseases can be traced back to factory farms, slaughterhouses, wildlife markets and illegal animal trade such as bushmeat. While markets selling wild and live animals have taken the brunt of the blame, the increasing global demand for meat is fuelling these outbreaks.
The conditions in which we keep farmed animals today, packed into filthy, overcrowded sheds, standing on top of each other and in their own faeces, physically stressed, pushed to the limit – an ideal breeding ground for emerging viruses and antibiotic-resistant bacteria.
Scientists from China warn: “SARS-CoV is only an example of emerging infections that we are going to face. In coming years, more cross-species infections are expected to happen. Factors influencing the chance of emergence of zoonotic infections are complex; and population density, ecology and proximity between animals and humans probably play a certain role”.
The global number of cases of Covid-19 has exceeded 700 million with over seven million deaths. Most of the world has gone through lockdown, experiencing restrictive measures usually only seen during wartime. Writing in The DailyTelegraph, Adjunct Professor of Global Health at the Duke Global Health Institute, Dr Jonathan Quick, says: “Traditional Chinese wet markets remain a threat to global health. China’s political and public health leaders must not fall into the cycle of short-lived commitments and long-term complacency following high-profile epidemics”.
But it’s not just wet markets, factory farming is just as much to blame. Not only are we decimating wild landscapes to clear the way for more intensively farmed animals, we are enclosing ever-increasing numbers of animals in filthy, overcrowded conditions, killing wild animals or caging them and sending them to market – all for the sake of our hunger for meat. Invading and disrupting ecosystems will inevitably shake viruses loose from their natural hosts just as factory farms are giving rise to superbugs. It’s time we listened to the warnings and put a halt to factory farming and wildlife markets.
The next bird flu outbreak could become a pandemic on a similar scale – chicken isn’t cheap if it costs thousands of lives and leads to a global recession.
Juliet Gellatley, founder and director of Viva! and zoologist says: “We must have a societal shift in the way we view animals, the environment and our diets. We must stop eating animals. It is time to finally make the connection between animal agriculture and environmental destruction, antibiotic resistance and disease outbreak. We must stop tearing down forests to make way for animal farming or to grow animal feed. We must protect ecosystems and prioritise the safety and freedom of wild animals, leaving them to live their lives away from human contact. If we don’t take urgent and far-reaching action now, eating animals will be the death of us”.
Stop factory farming – it’s time to go vegan!
Find out more about zoonotic diseases and how we can stop them
-
Covid
Covid-19 – what you need to know About Covid-19 Covid-19 caused a global health emergency and wreaked havoc across the world. It locked down entire countries and pushed healthcare services to the…
-
Mpox
Mpox (previously known as monkeypox) is a zoonotic infectious disease – transmitted to humans from animals. The symptoms are similar to those seen in people with smallpox, although less severe. If…